Home: Christchurch, NZ
Field role: Medical Team Leader; Emergency Training Focal Point/Doctor
Médecins Sans Frontières experience:
Field-based trainer, Geneva, 2017-2019, and eight field placements, including—
- Medical Team Leader, Afghanistan, 2020
- Emergency Room Trainer, Iraq, 2020
- Medical Activity Manager, Lebanon, 2020 and Syria, 2017
- Emergency Doctor, South Sudan and
- Mediterranean Search and Rescue, 2016
“It’s important to keep looking outwards”
Tell us about your career background.
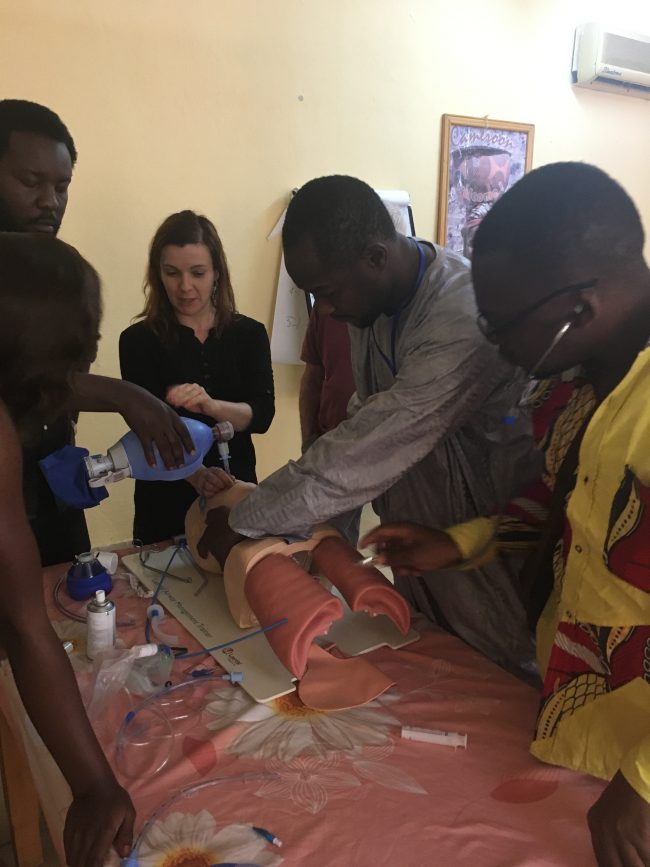
I worked as a doctor in the UK, New Zealand and Australia. I also spent time in Antarctica and Nepal practising wilderness medicine, which is medical care delivered in remote and resource limited environments like the poles, mountains or desert. I’d been interested in working with Médecins Sans Frontières for a long time, and after moving to New Zealand I joined through the Sydney office and went on my first assignment in 2009, to a trauma hospital in Nigeria.
You’ve now done eight field placements. Could you share any highlights?
My Médecins Sans Frontières career has taken varied directions, from starting as an emergency doctor, to later training, managerial and planning positions. I spent two years based in Geneva, flying to projects to run trainings for our teams in trauma and emergency care and mass casualty management. It was a great opportunity to work alongside lots of different colleagues, with a common goal of improving the quality of care for patients. I worked mainly in countries affected by conflict, including Iraq, Syria, Ukraine, Niger and Cameroon.
The most important thing I’ve learnt from training is to think about what information you’d like to share, but to then really listen to what the needs of the staff are, and make sure these two things match. Often there are major issues which impact people’s ability to deliver care, such as insecurity, overcrowding of health facilities and a lack of resources. You need to be mindful of what’s realistic, but with a careful approach it’s always possible to improve something.
What’s something people might not expect about your work?
Highly technical, complicated medicine can often steal the limelight, but simple interventions also save lives. Doing the basics well, in an organised way, can make a huge improvement in a trauma or mass casualty situation. This applies to medical care, and to organisation of workspaces: turning a bed head-to-wall, to allow doctors and nurses to focus on a patient in a crowded emergency ward; setting up a good resuscitation trolley or trauma kit; or having a clean work space. It’s a bit like extreme home makeover sometimes! These changes help make a chaotic and out-of-control situation easier to manage, which makes for better outcomes for patients and an improved working environment for staff.
Having worked as an emergency doctor, I know the emotional toll treating very sick or critical patients can take, so as a trainer I work with the staff in the project to troubleshoot, try new ideas and boost their confidence in putting them into practice. I learn a lot from my colleagues in the process.
Do you have any advice for others interested in a similar role with Médecins Sans Frontières?
It’s important to develop flexibility and resilience, especially if you want to commit long-term. You have to be able to cope with frequent changes, not only in terms of different geographical and cultural settings but also in the type of work. It helps to be open to all opportunities, and to keep your personal life as simple as possible! I rely on a strong international network of family and friends, and a commitment to the work.
What’s next for you?
Right now I’m working from NZ with a Médecins Sans Frontières medical unit based in Berlin, on an initiative to develop multimedia education tools for use in our programs. With COVID-19, we’ve had to look at different ways to deliver training resources to projects when in-person visits aren’t possible. I was grateful to work overseas throughout 2020, in Afghanistan, Lebanon and Iraq. This year will bring new challenges between COVID-19 and other crises, and although it can be difficult at these times it is still so important to keep looking outwards and to continue humanitarian support.
Who: Dr Rachel Tullet
What: Field Based Trainer
Where: Médecins Sans Frontières
To Find Out More Click Here
Share "MSF Profile with Dr Rachel Tullet"
Copy